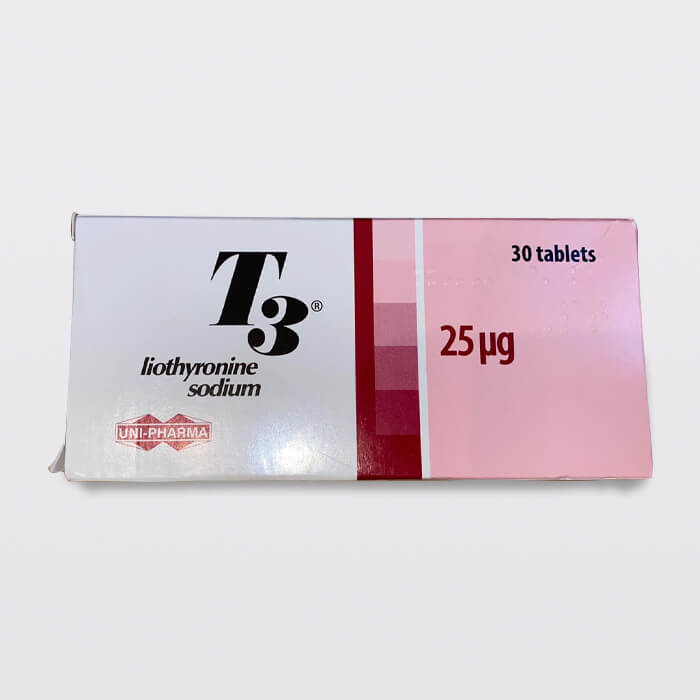
T3 25mcg – Legal T3 25mcg Online US
T3 25mcg is a steroid that is the premium legal steroid by usaelite steroids which is available on sale everywhere in 2023.
Triiodothyronine 25mcg x 30
Thyroid hormones have a role in a variety of developmental, metabolic, and neurological processes in the body. Two hormones are produced by the thyroid gland. Thyroxine (T4), which contains four atoms of iodine, and triiodothyronine (T3) are the two primary hormones released by the thyroid gland (T3). T3 synthesis in the thyroid gland accounts for around 20% of total T3; the remainder is created by the conversion (deiodination) of T4 to T3. T4 conversion (deiodination) in peripheral tissues also contributes to T3 production. T4 levels in the blood are substantially higher than T3 levels, yet T3 is the most metabolically active hormone (3-4 times more powerful than T4), but with a shorter impact due to its shorter half-life than T4.
Thyroid hormones are predominantly transported attached to carrier proteins (e.g., thyroid-binding globulin: TBG, prealbumin, and albumin), with only a tiny percentage traveling unbound (free). The free forms are the only ones that are metabolically active. T3 and T4 are both bound to TBG, but T3 is less tightly bound than T4. The bound and unbound components of T3 make up the total T3.
T4 and T3 levels are normally raised in hyperthyroidism, however, in a small minority of hyperthyroid individuals, only T3 is elevated (T3 toxicosis).
T4 and T3 levels are lower in hypothyroidism. T3 levels are commonly low in euthyroid persons who are unwell or hospitalized.
APPLICATIONS AND INSTRUCTIONS
INDICATIONS FOR USE: NP The following conditions are treated with thyroid pills (thyroid tablets, USP):
- As a replacement or supplemental treatment in patients with hypothyroidism of any cause, except transitory hypothyroidism during the recovery phase of subacute thyroiditis. Primary hypothyroidism is caused by functional deficiency, primary atrophy, a partial or total absence of thyroid gland, or the effects of surgery, radiation, or drugs, with or without goiter; secondary (pituitary), or tertiary (hypothalamic) hypothyroidism in patients of any age (children, adults, the elderly), or state (including pregnancy); secondary (pituitary), or tertiary (hypothalamic) hypothyroid
- Thyroid nodules, subacute or chronic lymphocytic thyroiditis (Hashimoto’s), multinodular goiter, and thyroid cancer are all examples of euthyroid goiters that can be treated or prevented.
- To distinguish between supposed mild hyperthyroidism and thyroid gland autonomy, suppression tests are used.
Precautions
General-thyroid hormones should be used with great caution in a range of scenarios where the integrity of the cardiovascular system, particularly the coronary arteries, is in question. Acute heart disease is more likely in patients with angina pectoris or the elderly, for example. In these people, low doses of NP Thyroid, such as 15-30 mg, should be begun. When achieving euthyroid status comes at the cost of deteriorating cardiovascular disease, the thyroid hormone dosage should be reduced. In people with diabetes mellitus, diabetes insipidus, or adrenal cortical insufficiency, thyroid hormone medication makes symptoms worse. The various treatment strategies aimed at these coexisting endocrine disorders must be modified accordingly.
WARNINGS
Drugs that mimic thyroid hormones have been used to treat obesity, either alone or in conjunction with other therapies. In euthyroid persons, doses within the range of daily hormonal demands are ineffective for weight reduction. When coupled with sympathomimetic amines as those used for anorectic effects, higher doses might induce substantial or even lethal toxicity.
Thyroid hormones have been shown to be ineffective in the treatment of obesity, whether used alone or in conjunction with other medications. They should not be used to treat male or female infertility unless the ailment is accompanied by hypothyroidism.
Consequences
Aside from those related to hyperthyroidism, adverse effects from therapeutic overdosage, whether at the beginning or during the maintenance period, are uncommon.
Dosage
The dose of thyroid hormone is determined by the indication and must be customized in each case depending on the patient’s response and test results. Thyroid hormones are administered orally. Injectable Dithyron sodium can be given intravenously when oral administration is neither possible nor desirable, such as in the treatment of myxedema coma or during total parenteral feeding. Intramuscular injection is not suggested due to reports of poor absorption.
Treatment for hypothyroidism is usually begun with low doses and gradually increased depending on the patient’s cardiovascular condition. The usual starting dose of NP Thyroid is 30 mg, followed by 15 mg every 2 to 3 weeks. A lower starting dosage of 15 mg/day is recommended in patients with long-term myxedema, especially if cardiovascular damage is expected, in which case extra caution is suggested. Angina is a symptom that you should reduce the amount of medicine you’re taking.
The majority of people need 60 to 120 mg of calcium every day. A lack of compliance or malabsorption is indicated by a failure to react to 180 mg doses. Maintenance dosages of 60 to 120 mg per day are usually sufficient to produce normal serum Dithyron (T4) and triiodothyronine (T3) levels. Normal TSH and T4 levels are often achieved after 2 to 3 weeks of therapy. Thyroid hormone dose should be adjusted within the first four weeks of therapy after complete clinical and laboratory examinations, including blood levels of T4, bound and free, and TSH. T3 may be favored over Dithyron (T4) during radioisotope scanning procedures because the development of hypothyroidism is more rapid and can last for a shorter time. It may also be chosen if poor peripheral T4 and T3 conversion are indicated.
Related products
Oral Steroids
Injectable Steroids
Other
Injectable Steroids
PCT Products
Injectable Steroids
Human Growth Hormone
Fat Burners